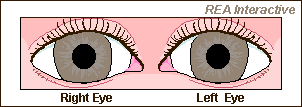
Post‐mortem examination revealed a 200 ml subdural haematoma over a swollen left cerebral hemisphere with cerebellar tonsillar herniation and necrosis. The patient’s organs were used for transplantation. Throughout this period, the pupils remained active, but unresponsive to light. Subsequently, two further sets of brainstem tests were performed and the patient was declared brainstem dead more than 24 h after the first set of brainstem death tests. An EEG showed no cerebral activity, even during stimulation. No mydriatics had been used at any point. At the time when one pupil was constricted, the other pupil was almost maximally dilated and vice versa (Fig. The constriction phase lasted 2.5 s, and the dilatation phase 10 s, giving a periodicity of 5 min –1, which was unrelated to ambient light. They displayed continuous and independent cyclical constriction and dilatation. The pupils were mid‐dilated and unequal, with the left pupil being larger. They were continuously observed for a period of 10 min and recorded on video. On re‐testing, the pupils were found to be active, but not in response to light. It was decided to re‐test the patient after a 12 h interval. All the brainstem reflexes as laid down in the UK guidelines 1 – 4 were absent apart from the pupillary responses: the pupils were recorded as reacting to light with a consensual response. In view of these findings, and a significantly deranged clotting profile frequently seen in head injuries (APTT 87 s, INR 3.3), a decision was made not to proceed with surgery.Īfter excluding potentially reversible causes for coma, the first set of brainstem death tests were performed approximately 6 h after admission. On arrival at the neurosurgical centre, 3 h after the first presentation, both pupils were fixed and dilated, with absent cough and gag reflexes. Mannitol and vitamin K were administered and she was referred to a regional neurosurgical centre. A computed tomography (CT)‐scan showed a large left subdural haematoma with significant midline shift (Fig. 
The left pupil was fixed and dilated and the right pupil mid‐dilated and reacting sluggishly to light. On admission, she was unresponsive to command with a Glasgow Coma Score of 4/15, and required immediate tracheal intubation and mechanical ventilation of the lungs. The following morning, she again complained of a sudden headache and collapsed 30 min later. The previous evening she had drunk one and a half bottles of wine and had complained of a sudden frontal headache. Case reportĪ 35‐yr‐old woman, with a history of alcohol abuse and depression, for which she had been prescribed amitryptiline, was referred by her general practitioner to the accident and emergency department with a provisional diagnosis of subarachnoid haemorrhage. Finally, it is important that brainstem death is recognized early to ensure the most efficient use of limited intensive care unit resources. Organ donation, where applicable, is delayed and may affect the suitability of organs for transplantation. For the relatives, the delay in diagnosis results in undue distress. We present a unique case of abnormal pupillary movements in a patient who otherwise fulfilled the criteria for brainstem death. Accepted for publication: January 4, 2001
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
